Abstract
Background
While smoking and genetic predisposition are known to confer an increased risk of lung diseases, less is known about the socioeconomic determinants of respiratory health. Disadvantages experienced at the neighborhood level may contribute to poor lung outcomes.
Objective
To quantify the impact of neighborhood disadvantage on respiratory outcomes in a general population cohort.
Methods
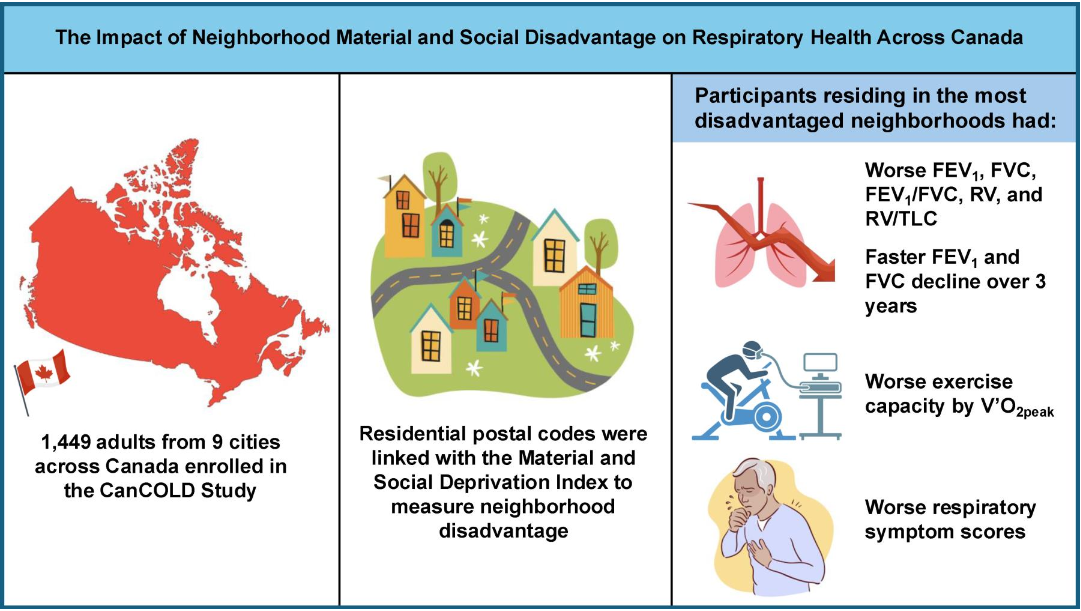
1449 adults enrolled in the Canadian Cohort Obstructive Lung Disease (CanCOLD) Study were followed for three years with repeat pulmonary function and cardiopulmonary exercise testing. Chest computed tomographic (CT) imaging was obtained at baseline. The Material and Social Deprivation Index was used to measure neighborhood disadvantage. Regression models were used to quantify the association between neighborhood disadvantage and pulmonary function, peak exercise capacity, quantitative CT measures, respiratory symptom scores, respiratory-related exacerbation events, and mortality.
Results
When compared to individuals residing in neighborhoods with the highest privilege, those residing in the most materially and socially disadvantaged neighborhoods had significantly worse forced expiratory volume in 1 s (FEV1), forced vital capacity (FVC), FEV1/FVC, air trapping, peak exercise oxygen consumption, and respiratory symptoms (all p<0.05). Over a three-year period, they also had significantly worse FEV1 (β −20.960 mL·year−1, p=0.012) and FVC (β −25.635 mL·year−1, p=0.042) decline. There were no significant relationships between neighborhood disadvantage and quantitative CT measures, exacerbations, or mortality.
Conclusions
Residence in the most materially and socially disadvantaged neighborhood is associated with worse lung function and exercise outcomes, highlighting a population particularly vulnerable to chronic airways diseases.