Abstract
Background
There is limited and conflicting evidence on the impact of obstructive sleep apnoea (OSA) and its treatment with positive airway pressure (PAP) therapy on pulmonary hypertension (PH). Our research question was: does treatment of OSA and obesity hypoventilation syndrome (OHS) with PAP therapy improve pulmonary arterial pressures?
Methods
A systematic review and random effects meta-analysis was performed (PROSPERO: CRD42024595312). PubMed, Embase, Scopus, Web of Science, EBSCO, Cochrane Central Register of Controlled Trials (CENTRAL) and ClinicalTrials.gov were searched using the PRISMA (Preferred Reporting Items for Systematic reviews and Meta-Analyses) guidelines. Studies reporting pulmonary arterial pressure in patients with OSA and OHS pre- and post-PAP therapy were included. The primary outcome was post-PAP therapy change in pulmonary arterial pressures, with separate analyses on pulmonary arterial systolic pressure and mean pulmonary arterial pressure. Sensitivity analysis was performed to assess the impact of PAP therapy in patients with only OSA or OHS.
Results
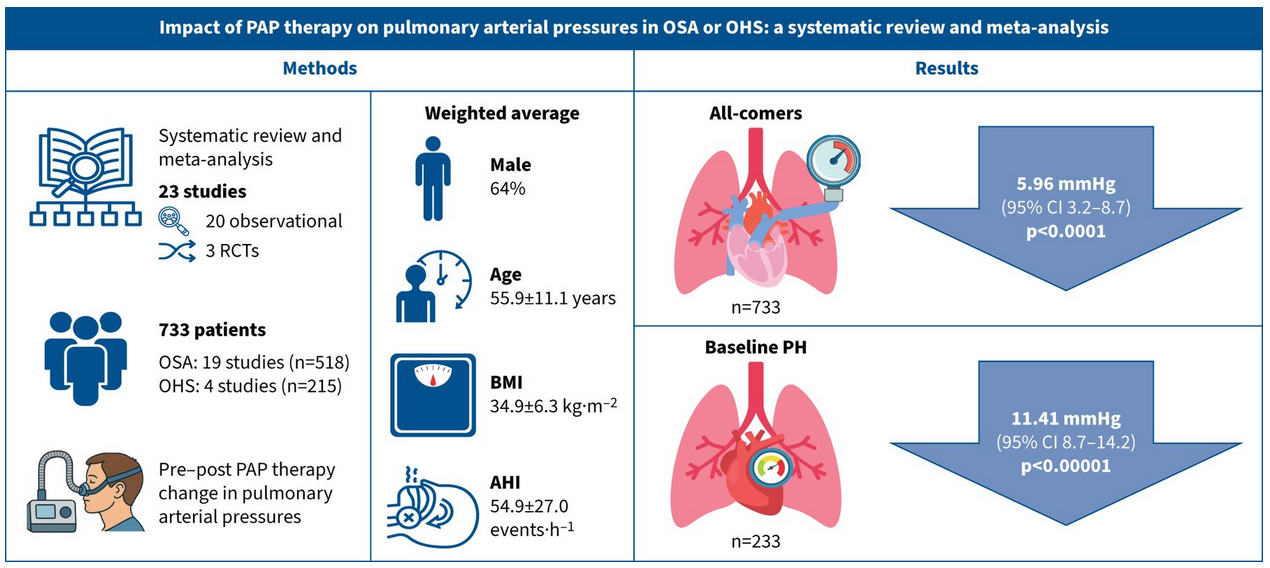
23 studies (20 observational and three randomised controlled trials) with 733 patients were included (19 with OSA (n=518) and four with OHS and concomitant OSA (n=215)). Most patients had severe OSA. PAP therapy was associated with a mean reduction in pulmonary arterial pressure of 5.96 (95% CI 3.20–8.73) mmHg; p<0.0001. In patients with baseline PH (n=233), the reduction was 11.41 (95% CI 8.66–14.15) mmHg; p<0.00001. The beneficial effect of PAP therapy was similar in OSA and OHS. There was no sex difference in the impact of PAP therapy. Heterogeneity was high across studies (I2>85%), reflecting differences in study design, patient populations and methodologies.
Conclusions
PAP therapy reduces pulmonary arterial pressures in patients with mostly severe OSA or OHS, with a more pronounced effect in those with baseline PH. As such, our findings may not apply to patients with milder degrees of OSA. While reductions in pulmonary arterial pressures were observed in all groups, the low certainty necessitates cautious application of these findings in clinical practice.