Praveen Govender, Yvette C. Cozier
European Respiratory Journal 2020 56: 2002376; DOI: 10.1183/13993003.02376-2020
Sarcoidosis patients treated with immunosuppressants have a higher risk of serious, recurrent infection. The high morbidity and mortality associated with COVID-19 require a cautious re-evaluation of short- and long-term sarcoidosis treatments. https://bit.ly/2YwZ9wb
We are living in a historic event: a novel virus, severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), emerged in Wuhan, China at the end of 2019 and began its global circulation. By January 24, 2020, at least 830 cases and 26 fatalities were reported across Asia and the USA. 6 months later, there are more than 8 million confirmed cases of the disease associated with SARS-CoV-2, coronavirus disease 2019 (COVID-19), and over 430 000 reported deaths worldwide. The pandemic has exposed cracks in healthcare systems throughout the world and identified populations vulnerable for severe disease and poorer outcomes, including the elderly, “essential workers” of lower socioeconomic class, and residents of nursing homes. The Centers for Disease Control (CDC) also state that those with chronic lung disease, namely asthma and COPD, the obese, and those with “prolonged use of corticosteroids and other immune weakening medications” might be at increased risk for COVID-19 related illness.
Although not specifically named in the CDC report, the list of underlying conditions accurately describe many patients with sarcoidosis, a systemic granulomatous disease that frequently affects the lung. It should not be surprising, in this pandemic, that these patients, and their physicians, are anxiously wondering whether they are more susceptible to COVID-19 or whether they might have a more severe clinical course. Thus, the report from Rossides et al. in the current issue of the European Respiratory Journal, is timely. While not explicitly answering the question of susceptibility of sarcoidosis patients to COVID-19 infection, the paper addresses this important concern in general and highlights an under-researched area in sarcoidosis literature: risk of secondary infections.
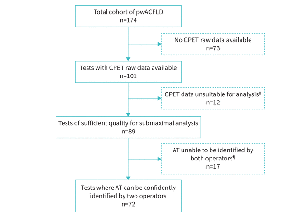
In their analysis, Rossides et al. examined hospitalisations and outpatient visits recorded in the Swedish National Patient Register to determine risk of serious hospitalised infections (SI), defined as a hospitalisation with an infectious disease as the primary discharge code (ICD-9). Over 8700 newly diagnosed sarcoidosis cases identified from 2003–2013 were matched to 86 000 general population controls on age, sex and residential location. Information on initial immunosuppressive therapy was available for 77% of the study population. They found that rates of SI and recurrent SI were 1.8-fold and 2.8-fold higher, respectively, in patients with sarcoidosis compared to the general population.
The relationship of sarcoidosis with infection is complex. Sarcoidosis is an exuberant or inappropriate granulomatous response to an undefined antigen(s). Among the many triggers known to cause granulomas, infection is the most common. Additionally, there are well-known infectious syndromes that complicate sarcoidosis (e.g. chronic pulmonary aspergillosis), but the incidence of this and other infectious complications is low. For example, Winterbauer and Kraemer reported opportunistic infections in five of 122 (4.1%) sarcoidosis patients in Seattle, WA, USA over a 7-year follow-up period. Further, there was no increased incidence of infection in comparison to normal controls, despite 71% of the patients having pulmonary involvement and 39% being on steroids. A retrospective record review by Baughman and Lower of clinic-based sarcoidosis patients found that only 7 out of 753 (0.9%) developed fungal infections over an 18-month period. In 2017, a hospital-based, retrospective cohort study of 585 French sarcoidosis patients, estimated a 5% frequency of severe infections (i.e. resulting in hospitalisation or death) over an 8-year (median) follow-up. In accordance with the findings of Winterbauer and Kraemer, the low frequency of infection observed in the latter two studies was in spite of high usage of corticosteroid therapy: 100% and 82% , respectively.
Conversely, results from a retrospective case–cohort study in Olmstead County, MN, USA from 1976 to 2013, suggested a diagnosis of sarcoidosis conferred a higher risk of infection requiring hospitalisation (hazard ratio (HR) 2.00, 95% CI 1.33–6.90). Use of steroids was a significant predictor of hospitalised infection; the hazard ratios for daily dosages of ≤10 mg and >10 mg were 3.03 and 4.48, respectively.
The current paper by Rossides et al. re-emphasises this latter observation; the negative impact of therapy. Immunosuppressive therapy is recommended, according to Wells's Law, for impaired quality of life or fear of danger (i.e. threatened organ failure). Corticosteroids are considered first line of treatment due to their ability to rapidly suppress granulomatous inflammation. Patients can relapse upon withdrawal, thus these agents are often prescribed for prolonged periods resulting in side-effects that can significantly impact quality of life. In the current analysis, risk of first SI was three-fold higher among those treated with immunosuppressants compared to those who were not. Although the indications for therapy, the length of therapy, and the cumulative dose of immunosuppressants used in the sarcoidosis cohort are unknown, prescribed treatment alone at the start of diagnosis was sufficient to increase one's risk for infection.
As the authors acknowledge, several study methods utilised impact the accuracy and validity of their results. These include the reliance on ICD coding to define both the study population and the outcome diagnosis, as well as use of prescriptions as surrogate for immunosuppressant use. Sarcoidosis encompasses heterogeneous clinical phenotypes and even patients with similar presentations have varied clinical courses. The paper does not address whether sarcoidosis in general or different phenotypes of sarcoidosis (e.g. Löfgren syndrome, non-Löfgren syndrome) result in worse clinical outcomes following hospitalisation. Equally, it does not address whether the identified increased risk of SI affects quality of life. A survey conducted by the European Lung Foundation Sarcoidosis Patient Advisory Group demonstrated that patients view quality of life as an important aspect of treatment that should be assessed and incorporated into clinical care. It is clear that further research in this area is needed.
So, should sarcoidosis patients be worried about SI? Yes and no. On the one hand, patients can be reassured that opportunistic infection is infrequent despite high corticosteroid use. This is shown in previous studies, and in the current study data, where after adjustment for having one or more healthcare visits in the 2 years prior to diagnosis, the risk of SI in untreated, newly diagnosed patients sarcoidosis appeared to be minimal (adjusted HR 1.03, 95% CI 0.88–1.22). On the other hand, risk for serious infections (i.e. hospitaliseable infection) is higher in treated, newly diagnosed patients.
Should sarcoidosis patients be worried about COVID-19 specifically? This is harder to answer. Approximately 2% of patients with COVID-19 have simultaneous pulmonary disease and experience worse outcomes than those without. Given the high morbidity and mortality associated with COVID-19 infection, there is concern that the risk–benefit calculation regarding immunosuppressive therapies for sarcoidosis may become unfavourable: continued treatment might increase risk of infection while therapeutic taper may increase symptoms. Despite this concern, it has yet to be established whether sarcoidosis is a risk for development of disease or for poorer outcomes.
In light of the COVID-19 pandemic, Sweiss et al. have issued an opinion statement stressing the importance of minimising the initial treatment dose of immunosuppression therapy, which is the standard, accepted practice in the management of sarcoidosis. They further call upon clinicians to taper existing patients to the lowest effective dose. While this may appear straightforward, disparity in socioeconomic status may make such adjustment difficult to achieve.
A recent paper from the USA by Harper et al. found an inverse association between socioeconomic status and long-term, steroid-related comorbid conditions among sarcoidosis patients. Lower socioeconomic status individuals in the USA may have limited ability to take time off from work for follow-up clinic visits, and additional costs associated with physician visits (e.g. transportation, insurance co-payments) may make multiple clinic visits burdensome. However, Sweden has a tax-funded, universally accessible healthcare system, therefore, it is not clear from the current analysis whether Swedish patients face similar impediments to care. Additionally, Sweden and the USA differ in terms of racial composition, healthcare access, and the distribution of chronic health conditions (e.g. obesity, type-2 diabetes).
Rossides et al. have helped us to understand generally the risk of serious hospitalised infections in newly diagnosed cases of sarcoidosis, and highlights that the initial decision to treat is important as it could have lasting harmful effects. The COVID-19 pandemic has exposed major social and financial fissures globally. Furthermore, recent events in the USA have amplified these fault lines. Racial and social disparities undergird much of contemporary American society, and to a different extent, societies around the globe. Since sarcoidosis disproportionately affects the lives of persons with low socioeconomic status and racial minorities (for example, African Americans/Blacks), the article by Rossides et al. also serves as a reminder that sarcoidosis straddles the historic convergence of the COVID-19 pandemic and exposure of societal inequality in healthcare outcomes.
Acknowledgement
We are grateful to Jeffrey Berman for his editorial feedback and mentorship.
Footnotes
-
Conflict of interest: P. Govender has nothing to disclose.
-
Conflict of interest: Y.C. Cozier has nothing to disclose.
-
Support statement: Y.C. Cozier is supported by the National Cancer Institute U01-CA164974, and the National Institute of Arthritis and Musculoskeletal and Skin Diseases R01 AR0573727. Funding information for this article has been deposited with the Crossref Funder Registry.
- Received June 17, 2020.
- Accepted June 21, 2020.
- Copyright ©ERS 2020